Impact Sante Afrique (ISA), together with Ghana’s National Malaria Elimination Programme, has launched a documentary series called #ProtectTheCure to show the real situation of malaria drug resistance in Africa.
The four-part series, produced by Boni Lab at Temple University with Normal Life Pictures Ltd, aims to get decision-makers and communities involved in protecting malaria medicines for future generations.
Through scientists, public health experts, and affected communities, the film explains what Artemisinin resistance is, why it matters, and what can be done to stop it.
Malaria continues to be one of the biggest health challenges in sub-Saharan Africa, affecting millions of families every year. In 2023, the WHO reported about 263 million malaria cases and 597,000 deaths worldwide, with Africa accounting for 95% of these deaths.
Besides the human toll, malaria puts huge pressure on health systems, slows economic growth, and affects the well-being of communities.
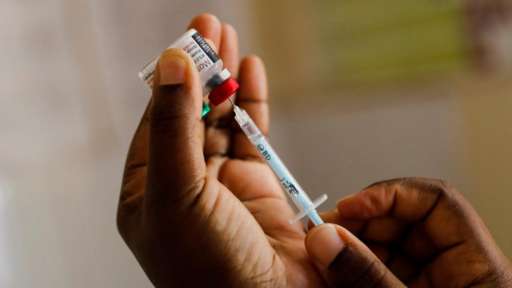
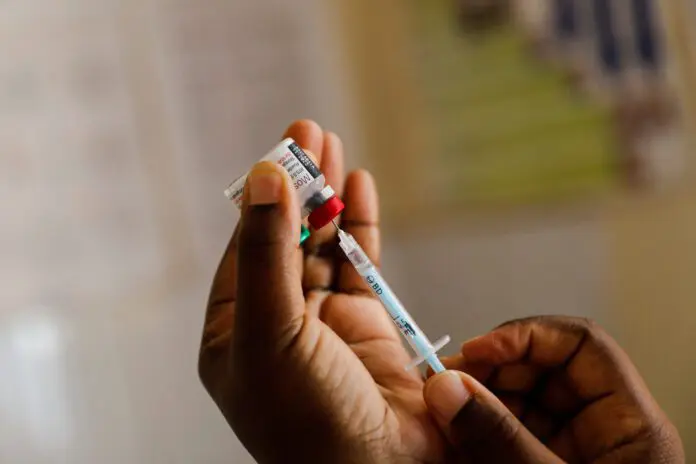
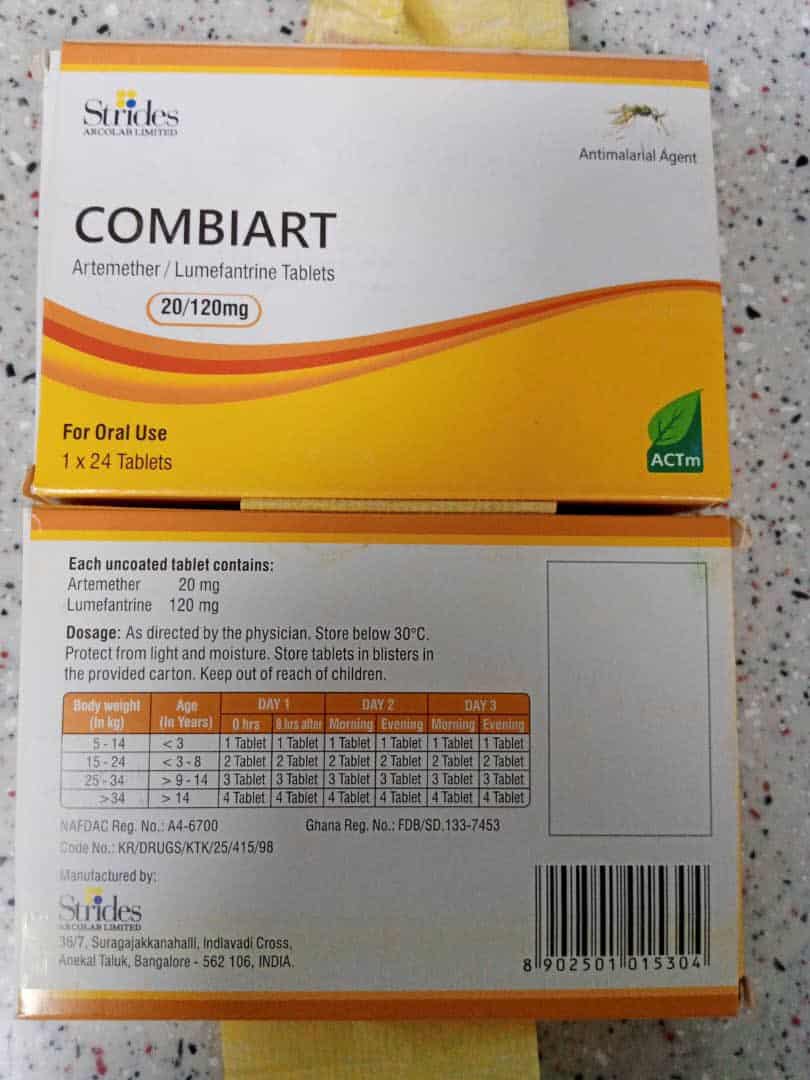
For the last 20 years, artemisinin-based combination therapies (ACTs) have greatly improved malaria control and saved millions of lives. But the rise of partial artemisinin resistance now threatens to undo this progress.
Dr Felicia Owusu-Antwi, WHO Ghana Officer for Malaria and Neglected Tropical Diseases, advised African countries to adopt multi-first-line therapy medicines to stop malaria drug resistance. She made the recommendation during a Regional dialogue on Malaria Drug Resistance in Africa, held alongside the International Conference on AIDS and Sexually Transmitted Infections in Africa (ICASA 2025).
She explained that the approach “involved making several different, effective ACTs available at the national level, rather than relying solely on a single option for the treatment of malaria on the continent.”
Dr Owusu-Antwi also said African countries must carry out studies to track how well their malaria medicines are working. She stressed that this is necessary because the medicines “were gradually becoming ineffective because the malaria parasites were learning to overcome them.”
She warned: “If we lose these ACTs, we lose our strongest line of defence. We will see more severe cases, more deaths, overcrowded health facilities, and higher out-of-pocket payments for households.”
Despite tools to detect resistance, many African countries struggle with surveillance due to a lack of funding. Dr Owusu-Antwi urged governments to take charge of malaria research, education, and monitoring, warning that “poor treatment adherence, self-medication, and the circulation of substandard drugs were worsening the threat.”
Dr Mark Nawaane, Chairman of the Parliamentary Select Committee on Health and a member of COPEMA, called on African governments to provide resources to fight malaria. He highlighted Ghana’s ongoing efforts, including destroying larvae, using treated bednets, and indoor spraying.
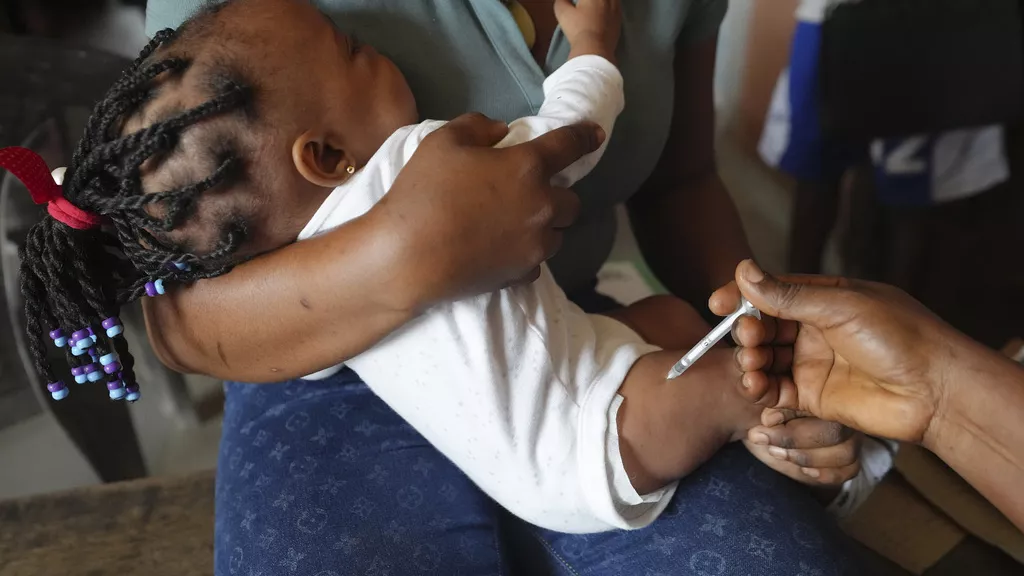
He added: “We are importing the drugs. And now there is even a vaccine to assist us, to vaccinate the children against malaria. But we need to keep up the tempo of the fight.”
Dr Nawaane also revealed that soon, malaria treatment under the government’s primary healthcare programme will be free: “When that happens, anybody suffering from malaria will not be sitting in the house; they will come to the health facilities. And as you know, when you start the treatment early, your resources will be better, and then there will not be any treatment failure.”
He said education in communities is ongoing to teach people how to respond when they have malaria.
Mrs Cecilia Senoo, Executive Director of Hope for Future Generations (HFFG), called for stronger collaboration with civil society, saying: “Malaria elimination cannot succeed when key partners are sidelined. Civil society, manufacturers, mothers, community leaders, and the media all have critical roles. We need innovative strategies for prevention and sustained education.”
She also urged the government to invest in malaria research and expand the malaria vaccination programme, stressing that Ghana should not depend solely on donor funding. Senoo called for greater involvement from the private sector, including mining companies.
Dr Hilarius Abiwu, Programme Manager at the National Malaria Elimination Programme, reassured that current malaria medicines in Ghana remain effective, with cure rates close to 100%. He emphasized that waiting to react is not a strategy, noting the need for early-warning systems and planning. He also revealed that Ghana is exploring triple-drug combinations to stay ahead of resistance.
The regional dialogue was organised in collaboration with the RBM Partnership to End Malaria, Medicines for Malaria Venture (MMV), Target Malaria, and Hope For Future Generations (HFFG).