The total confirmed cases of monkeypox (Mpox) in Ghana now stand at five hundred and sixty-five (565). The current update by the Ghana Health Service (GHS) follows the confirmation of 10 new cases recorded as of Thursday, September 18.
This reflects a surge from 519 confirmed cases reported on Thursday, September 11. On August 28, 21 new cases brought the total to 467, while on August 25, the Service reported 22 cases, which pushed the cumulative figure at the time to 446.
On August 20, 15 new cases were recorded, making the number at the time 424. Currently, there’s no patient on admission. As of August 14, four hundred and nine (409) total cases were confirmed after thirty-seven (37) new cases were recorded.
According to previous reports, twenty-six (26) new cases of infection were confirmed on August 11, increasing the total to 372, compared to 346 cases reported on August 7. However, the national death toll stands at two.
Unfortunately, all 16 regions have recorded cases of the disease so far in the country. The increasing number of cases in the country continues to raise concerns. In the meantime, the country can breathe a sigh of relief as 33,600 vaccines have been secured by the Health Ministry to strengthen Ghana’s fight against the monkeypox (Mpox) virus.
“This is another milestone in safeguarding the health and well being of our citizens,” the ministry said in a Facebook post.Months ago, the Ministry of Health received a significant boost in its fight against the ongoing Mpox outbreak following the donation of essential medical supplies and public health materials from the World Health Organization (WHO).
During a brief ceremony held at the Ministry, the WHO Regional Director for Africa, Professor Mohamed Yakub Janabi, reaffirmed the organization’s commitment to supporting Ghana’s public health response and acknowledged the country’s commendable leadership in managing the outbreak.
The donation, valued at USD 36,700, includes personal protective equipment (PPE) for frontline health workers, 780 GeneXpert cartridges to improve diagnostic capacity, and 9,000 risk communication posters along with 40 pull-up banners to support community sensitization efforts.
The PPE will help enhance infection prevention and control, while the GeneXpert cartridges are expected to facilitate rapid and accurate testing, particularly at decentralized levels.
The risk communication materials are aimed at promoting public awareness and behavioural change. The Minister for Health, Honourable Kwabena Mintah Akandoh, who received the items on behalf of the government, thanked the WHO for its continued support.
He indicated that Ghana is keen to adopt vaccines as part of its response strategy and called on the WHO to expedite assistance in that regard. He also encouraged the public to maintain good hygiene practices and to seek prompt medical attention if they experience symptoms such as fever, cough, headache, or skin rashes.
He noted that the Ministry remains committed to strengthening public health systems and working closely with partners to contain the outbreak and protect the health of all Ghanaians.
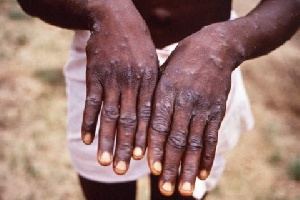
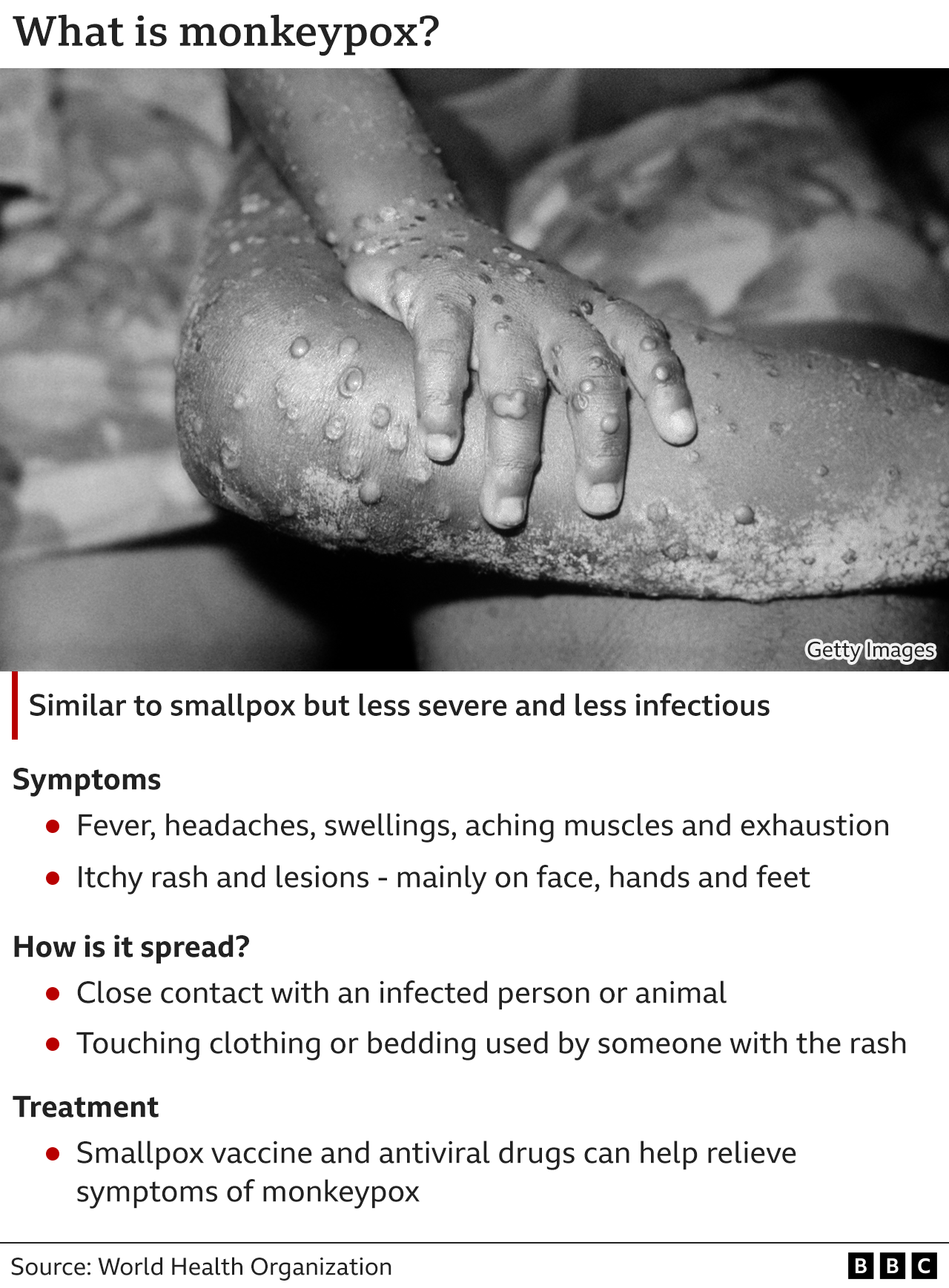
Health officials explained that the Mpox disease primarily spreads through direct contact with an infected individual. Common signs include fever, skin rashes, and swollen lymph nodes.
The Ghana Health Service is urging the public to avoid close interactions with symptomatic persons, maintain regular handwashing with soap and water, refrain from frequently touching the face, and use masks when caring for patients.
The Service added that it is closely monitoring the outbreak, conducting contact tracing, and strengthening public education with the support of regional health directorates.
Following the detection of twenty (20) new infections as of Wednesday, July 30, the Ghana Health Service (GHS) on Monday, July 27, reported the unfortunate demise of one of the individuals who had contracted the disease.
Since Ghana recorded its first Mpox case in June 2022, with five cases, this is the first time any of the infected persons has succumbed to the disease. In its regular updates, the Ghana Health Service noted that as of July 22, twenty-three (23) new cases were recorded, pushing the total confirmed cases to 257 at the time.
Ghana’s confirmed Mpox cases rose to 234 following the detection of sixteen (16) new cases as of July 18.The number of cases stood at 218 after twenty-one (21) new infections were detected as of July 14.
The Ghana Health Service reported 197 confirmed cases following the detection of eleven (11) new infections as of July 11.The Service, while revealing this information, described the trend as a gradual yet manageable increase and called for sustained public vigilance.
The country has seen a slight uptick in infections. Health officials, however, maintain that the overall situation remains under control. Although many cases are mild, early medical care is crucial to avoid complications.
In light of the growing Mpox cases, the GHS is boosting nationwide information campaigns to ensure citizens remain aware and cautious.
Preventive actions such as avoiding direct contact with sick individuals, practicing proper hygiene, and promptly seeking care when symptoms show are being emphasized.
Officials stress the importance of swift case detection and notification, with field teams and community health workers diligently monitoring developments.
The public is being encouraged to stay watchful, adhere to health precautions, and contribute to collective efforts to stop the virus from spreading.
The government is engaging international organizations for assistance in procuring vaccines to help curb the rising number of cases being reported.
The World Health Organization (WHO) in Ghana has provided laboratory PCR reagents to enhance the country’s diagnostic capacity. The donation was officially handed over to the Ghana Health Service (GHS) at the National Public Health Reference Laboratory.
Receiving the supplies on behalf of the GHS, Acting Deputy Director General Dr. Caroline Reindorf Amissah expressed gratitude for WHO’s ongoing logistical and technical support. “We promise from our end to do our bit, collaborate, go out there, and look for the cases to make sure that this is really brought under control,” she stated.
WHO Country Representative Dr. Fiona Braka emphasized that the organization hopes the reagents will enable rapid diagnosis and prompt public health responses. The supplies are capable of testing 3,400 suspected Mpox samples, and additional kits provided will allow clade determination for 625 confirmed positive cases.
Global Data
The monkeypox virus was first discovered in Denmark in 1958 in monkeys kept for research, according to the World Health Organization (WHO). A nine-month-old boy from the Democratic Republic of Congo in 1970 was the first person to contract the virus.
According to the World Health Organization, following the eradication of smallpox in 1980 and the end of smallpox vaccination worldwide, Mpox steadily emerged in central, east, and west Africa.
“Since then, mpox has been reported sporadically in central and east Africa (clade I) and west Africa (clade II). In 2003, an outbreak in the United States of America was linked to imported wild animals (clade II).
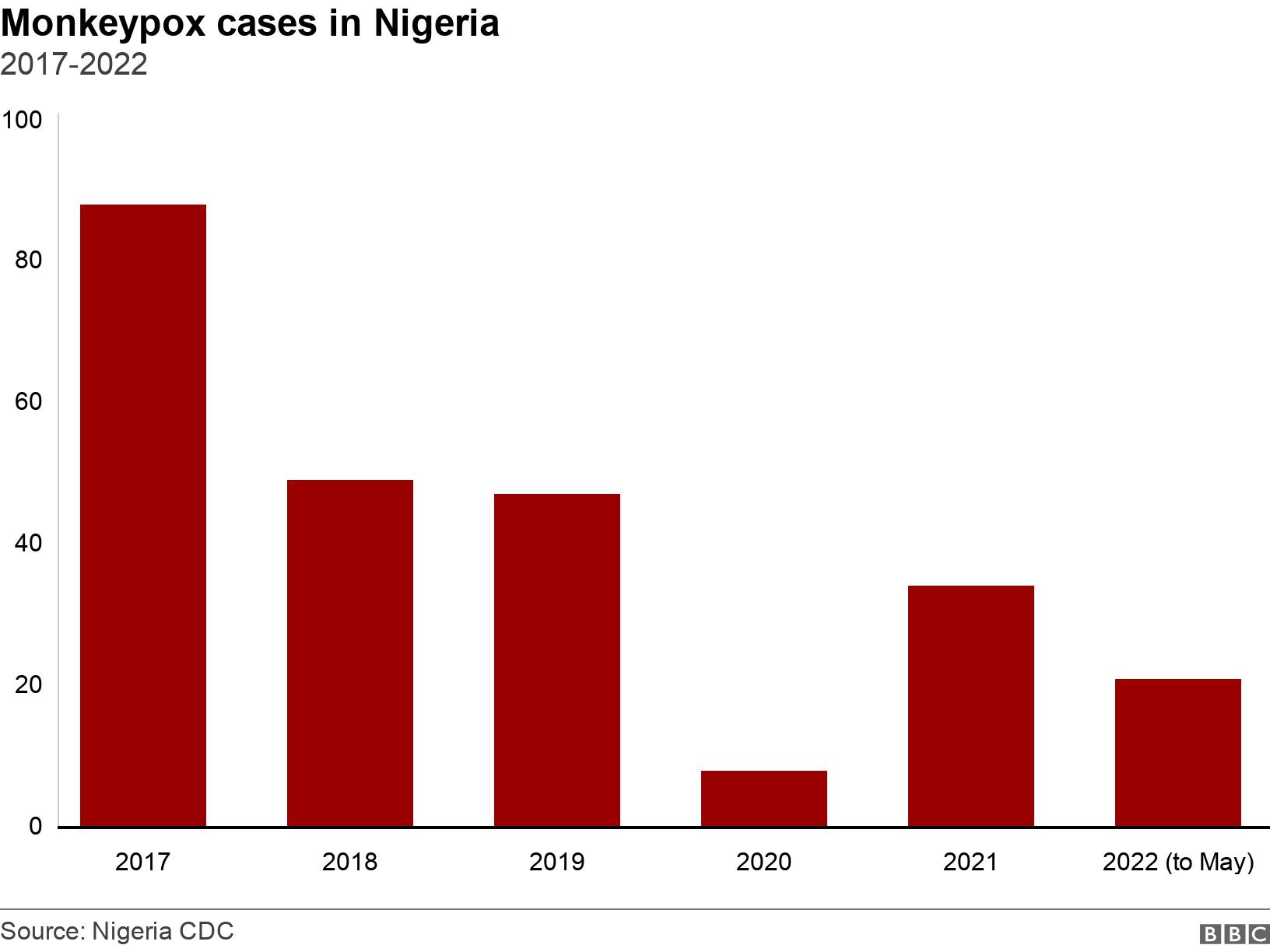
Since 2005, thousands of cases have been reported in the Democratic Republic of the Congo every year. In 2017, mpox re-emerged in Nigeria and continues to spread between people across the country and in travellers to other destinations,” the WHO reports.
In May 2022, an outbreak of Mpox appeared suddenly and rapidly spread across Europe, the Americas, and then all six WHO regions. Since 2022, there has also been an upsurge in Mpox cases and deaths in the Democratic Republic of the Congo.
In some areas of the country, a new offshoot of clade I, called clade Ib, has been spreading person-to-person. As of mid-2024, the clade has also been reported in other countries.
Over 120 countries have reported Mpox between January 2022 and August 2024, with over 100,000 laboratory-confirmed cases and more than 220 deaths among confirmed cases.
Following the meeting of the International Health Regulations (2005) Emergency Committee regarding the upsurge of Mpox in 2024, held on June 5, 2025, the World Health Organization stated that “Over the past 12 months, the majority of mpox cases have continued to be reported from the African continent, largely driven by outbreaks of MPXV clade Ib in East African countries, including the DRC, where clade Ia is co-circulating.
Sierra Leone, however, is experiencing a rapidly evolving outbreak, which, based on available genomic sequencing results, appears to be driven by MPXV clade IIb.
“Outside of the African region, there continues to be a steady report of monthly cases (between about 500 – 1000 monthly), from all regions, mostly reflecting ongoing circulation of MPXV clade IIb among men who have sex with men (MSM),” the WHO added.
WHO Director-General Dr. Tedros Adhanom Ghebreyesus has declared Mpox a Public Health Emergency of International Concern (PHEIC) twice. The first was in May 2022, and the second time was in August 2024.
The World Health Organization continues to work with member states and partners to prevent and respond to outbreaks of Mpox.
This includes coordinating research on vaccines and treatments, strengthening country health systems, and working to facilitate equitable access to vaccines, therapeutics, diagnostics, and other tools.